Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
Which type of search should you perform?
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
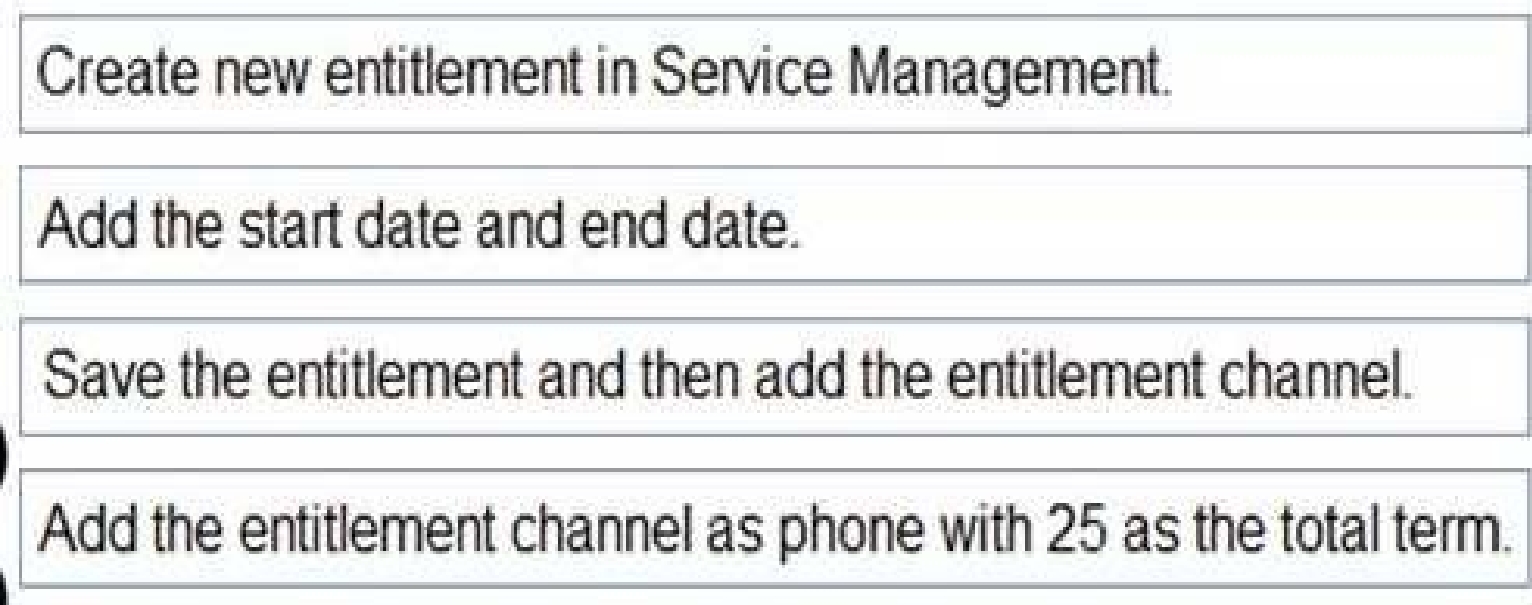
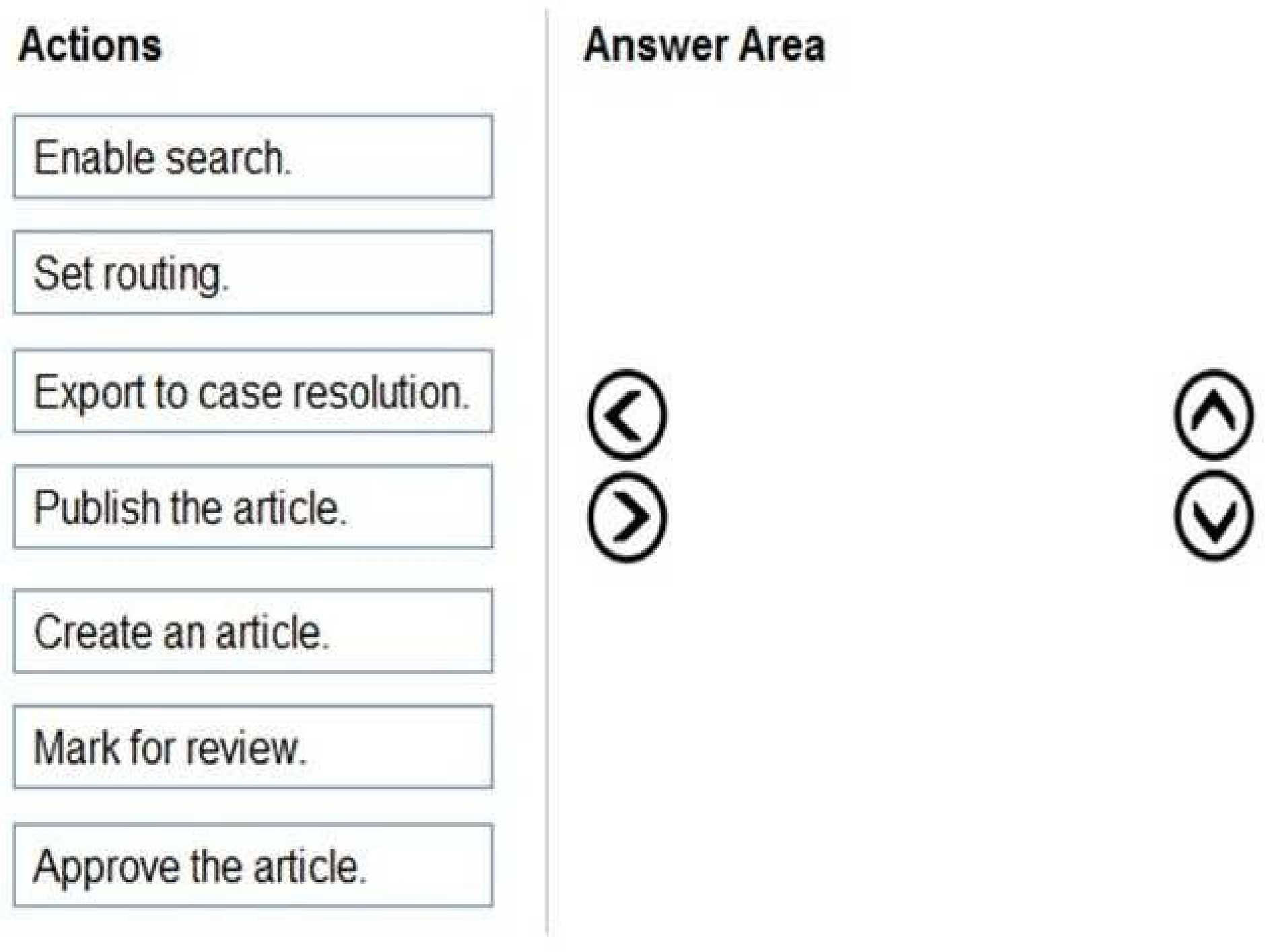
You need to configure the system to store answers about claims.
Which four actions should you perform in sequence? To answer, move all actions from the list to the
answer area and arrange them in the correct order.
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
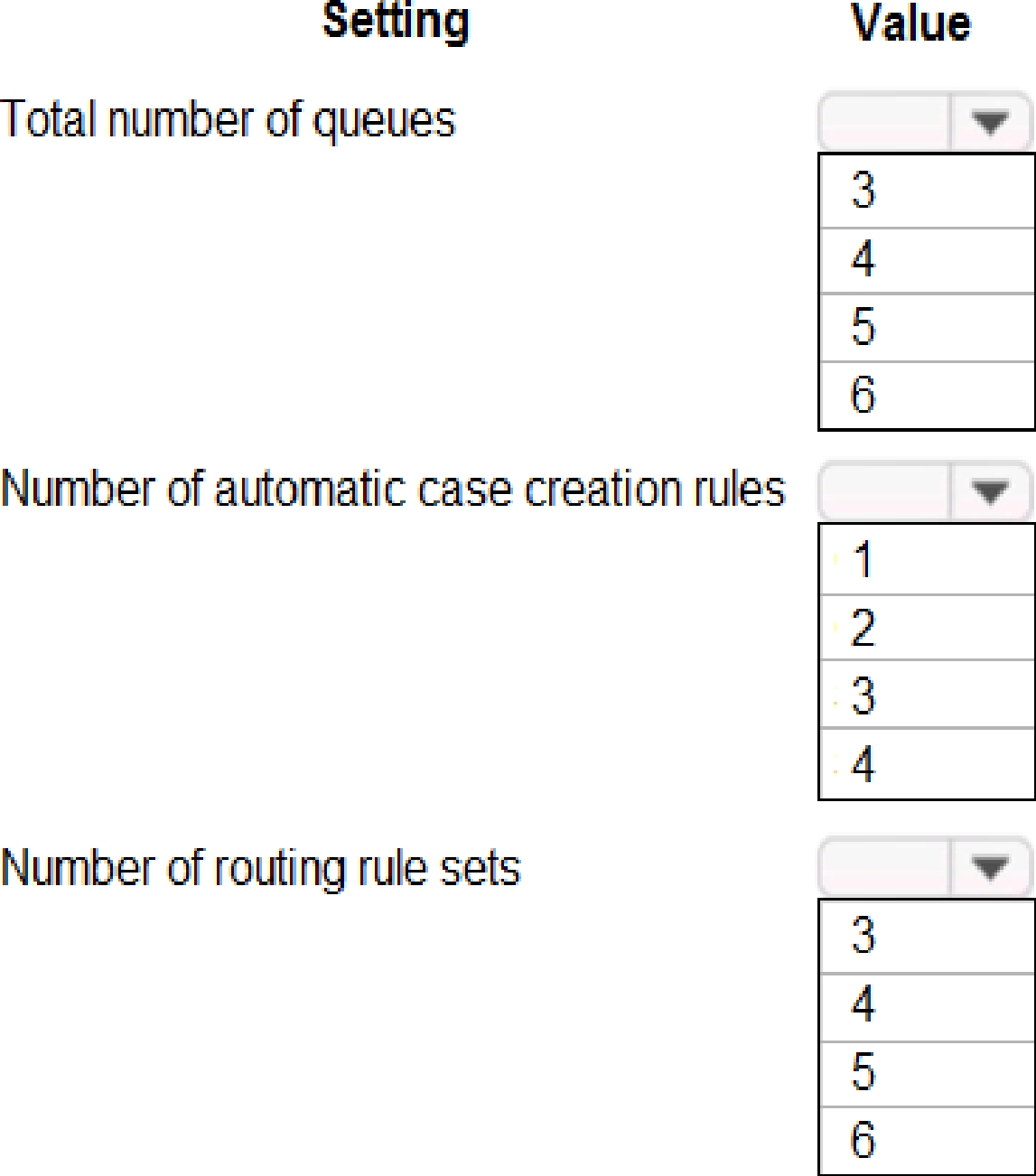
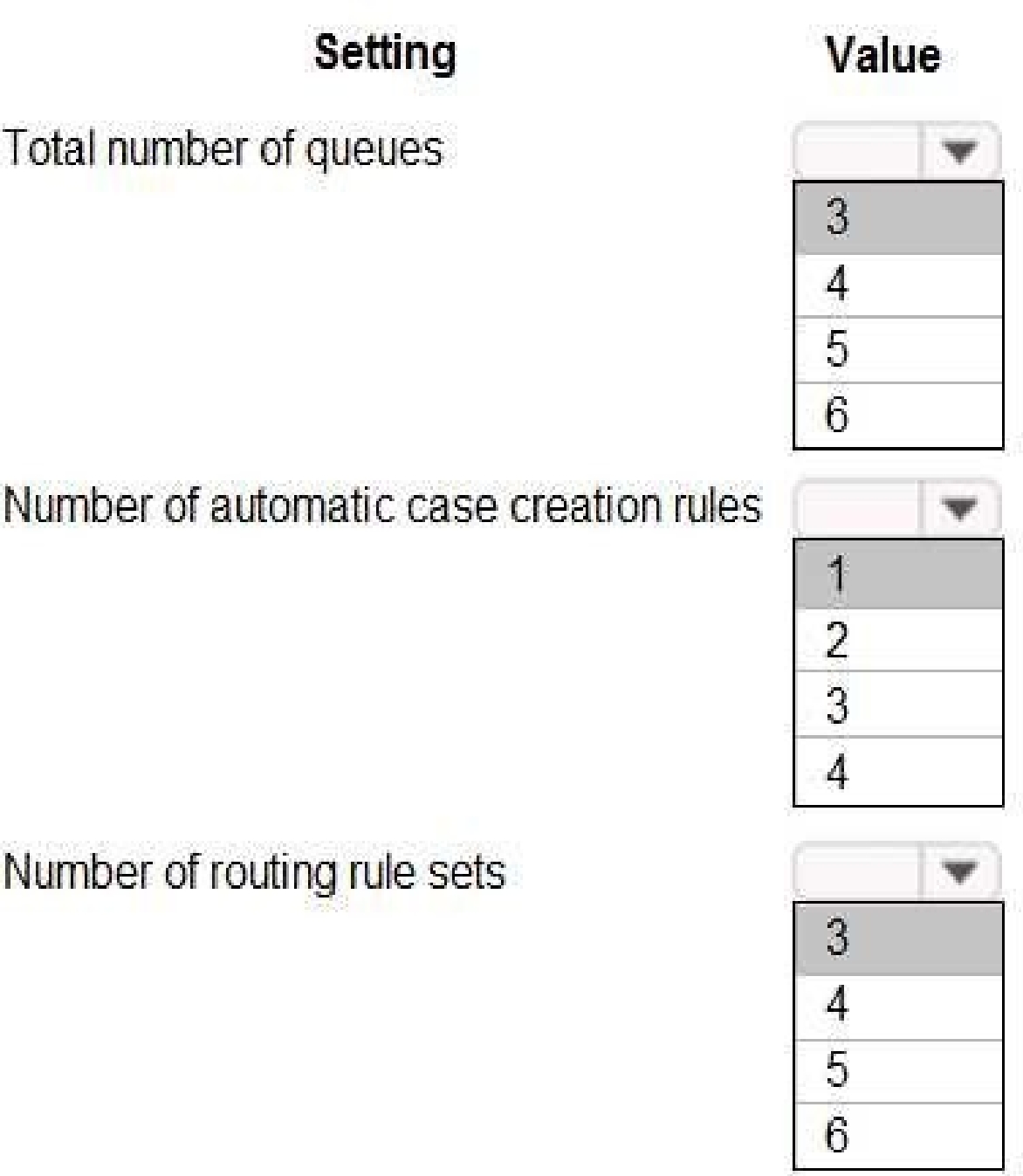
How should you configure the system? To answer, select the appropriate options in the answer area.
NOTE: Each correct selection is worth one point.


Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
What are two possible ways to achieve this goal? Each correct answer presents a complete solution.
NOTE: Each correct selection is worth one point.
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
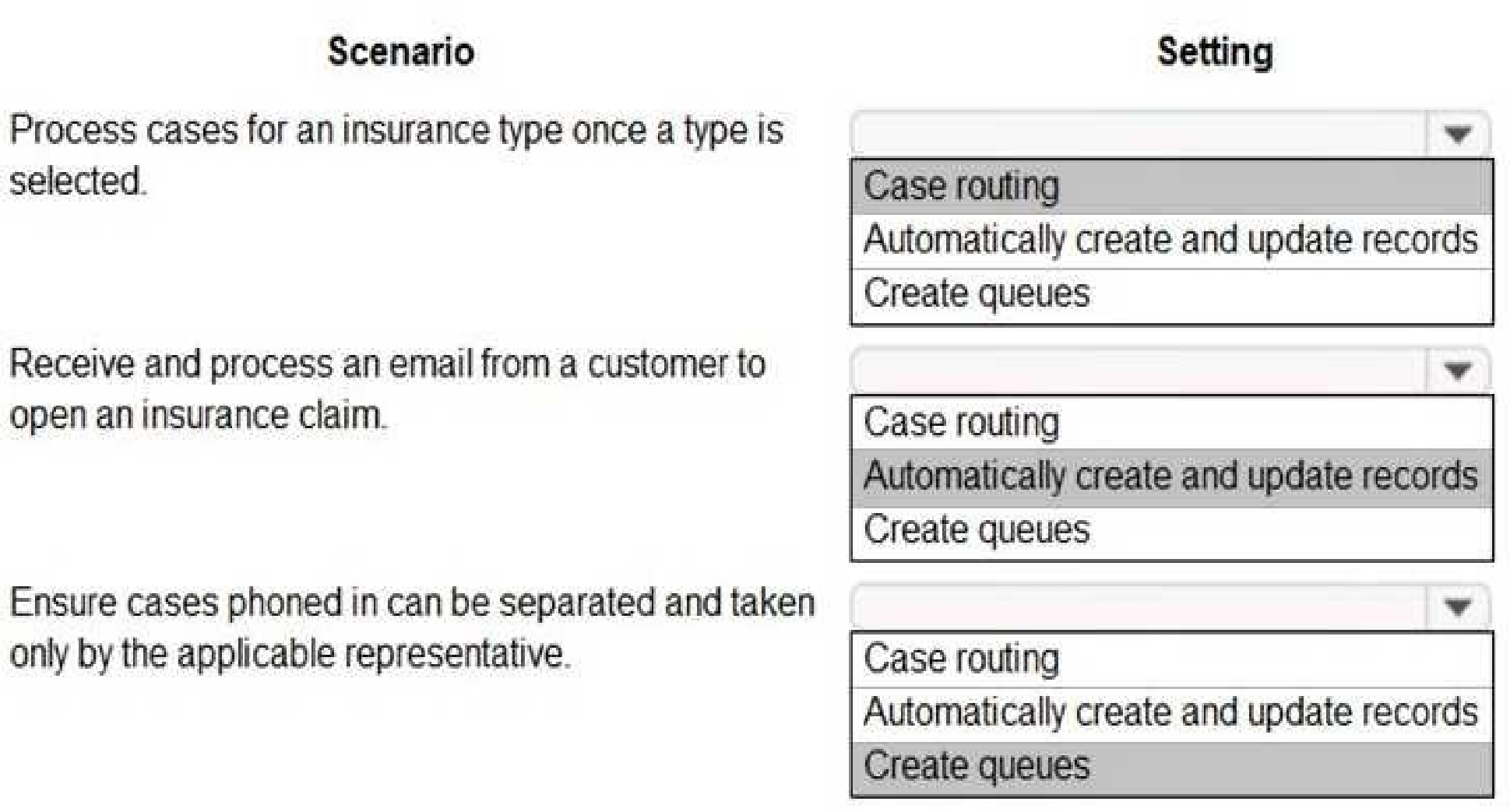
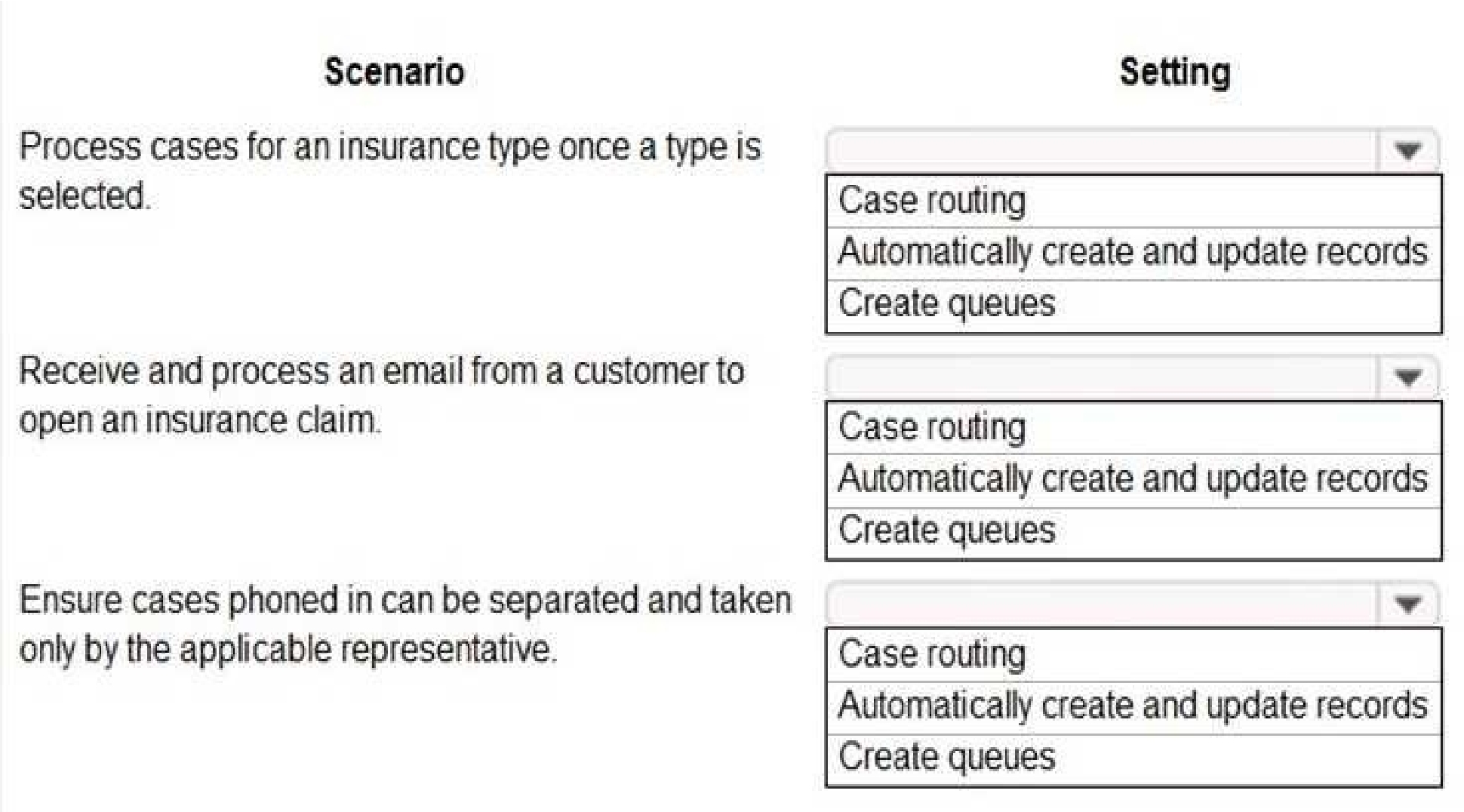
Which settings should you configure? To answer, select the appropriate options in the answer area.
NOTE: Each correct selection is worth one point.

Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
What should you configure?
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
You need to determine how many cases the customer has left on their entitlement.
How many cases are left?
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
Which three SLAs should you create? Each correct answer presents part of the solution.
NOTE: Each correct selection is worth one point.
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
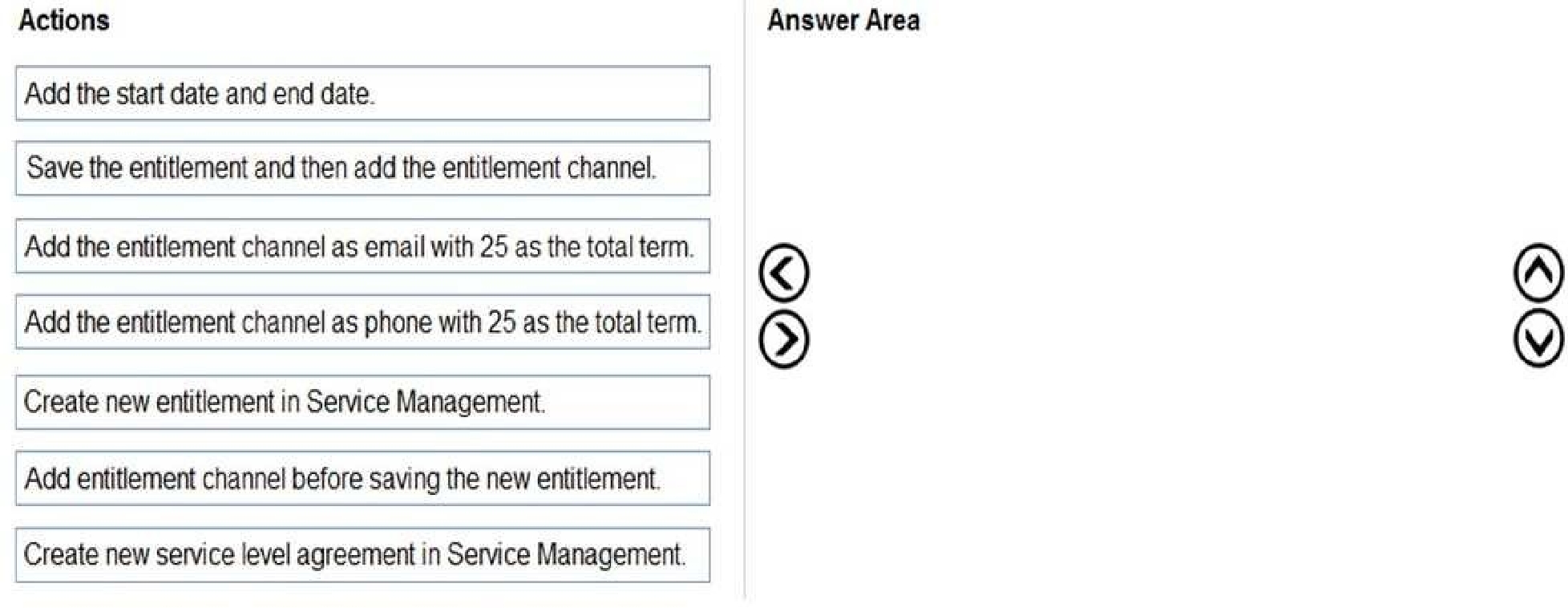
You need to ensure that customers cannot open more cases than they are allowed.
Which four actions should you perform in sequence? To answer, move the appropriate actions from
the list of actions to the answer area and arrange them in the correct order.
Quiz
Case Study
Overview
This is a case study. Case studies are not timed separately. You can use as much exam time as you
would like to complete each case. However, there may be additional case studies and sections on
this exam. You must manage your time to ensure that you are able to complete all questions included
on this exam in the time provided.
To answer the questions included in a case study, you will need to reference information that is
provided in the case study. Case studies might contain exhibits and other resources that provide
more information about the scenario that is described in the case study. Each question is
independent of the other questions in this case study.
At the end of this case study, a review screen will appear. This screen allows you to review your
answers and to make changes before you move to the next section of the exam. After you begin a
new section, you cannot return to this section.
To start the case study
To display the first question in this case study, click the Next button. Use the buttons in the left pane
to explore the content of the case study before you answer the questions. Clicking these buttons
displays information such as business requirements, existing environment, and problem statements.
If the case study has an All Information tab, note that the information displayed is identical to the
information displayed on the subsequent tabs. When you are ready to answer a question, click the
Question button to return to the question.
Background
Humongous Insurance is contracted to process all insurance claims for a health facility that accepts
the following types of health insurance:
Health maintenance organization (HMO)
Preferred-provider organization (PPO)
Gold
Cases are classified as new claims, claim disputes, and follow-ups. Each insured person is entitled to
open 25 new cases each calendar year.
Support representatives specialize by and process claims by insurance type.
Humongous Insurance currently accepts claims only by telephone. The call center is open from 06:00
GMT to 24:00 GMT daily. Call center staff work one of the following shifts: 06:00 GMT to 12:00 GMT,
12:00 GMT to 18:00 GMT, and 18:00 GMT to 24:00 GMT.
When a case is received by email, a staff member categorizes the case as email and closes the case
immediately.
Current environment
Humongous Insurance has three departments to handle claim types: HMO, PPO, and Gold.
The company uses handwritten forms to send claims information to the correct department.
Each department maintains a workbook to record calls received.
Requirements. Support desk
Configure the system to track the number of insurance claims filed each year.
Categorize claims by type as they are opened.
Configure the system to track staff responsiveness to service-level agreements (SLAs).
Ensure that business hours reflect the hours that support staff are scheduled.
Requirements. Case handling
All new cases must be automatically placed into a queue based on insurance type after the type is
selected.
All insurance types need to be automatically moved to the proper queue when the subject is picked.
All cases must be created and closed immediately when received.
The status reason must be set to Email Sent or Phone Call.
Information must be restricted by insurance and phone call type.
Managers must be alerted when customers reach their limit of 25 cases for the year.
Changes to cases must not be counted against entitlements until the case is closed.
Requirements. Disputes
Claim disputes must be categorized as low priority.
The status for all disputed cases must be set to Review by a Manager before a disputed case may be
closed.
Requirements. Knowledge base
A knowledge base must be used as a repository for all answers.
Representatives must be able to search the knowledge base when opening a new case for similar
claims.
Representatives must be able to search across all entities at all times.
Searches must check any field in the entity for matches in a single search.
Searches must return results in a single list and sort the list so that the most relevant results appear
at the top of the list.
Representatives must be able to link the knowledge base to cases when applicable.
Representatives must create a new knowledge base article if an answer is not found in the existing
knowledge base.
Representatives must be able to use SQL-like syntax to search the knowledge base.
Requirements. Service-level agreements
When a customer calls to open a claim, the company must respond to the caller within the following
time frames:

Requirements. Alerts
Cases must be flagged when they are past the SLA threshold.
An email alert must be sent to the manager to indicate an SLA noncompliance.
An email alert must be sent to representatives for SLA violations as follows: HMO 2 hours prior and
PPO 1 hour prior.
Send an email alert to support managers when disputes are ready to be closed.
Send an email alert to customers when cases are closed.
Requirements. Issues
The current process is all manual and not efficient.
There is no easy way to determine whether the company is meeting its SLAs.
Representatives are often inconsistent regarding how they handle customers and answer customer
questions.
There is no accountability for any of the representatives who take calls.
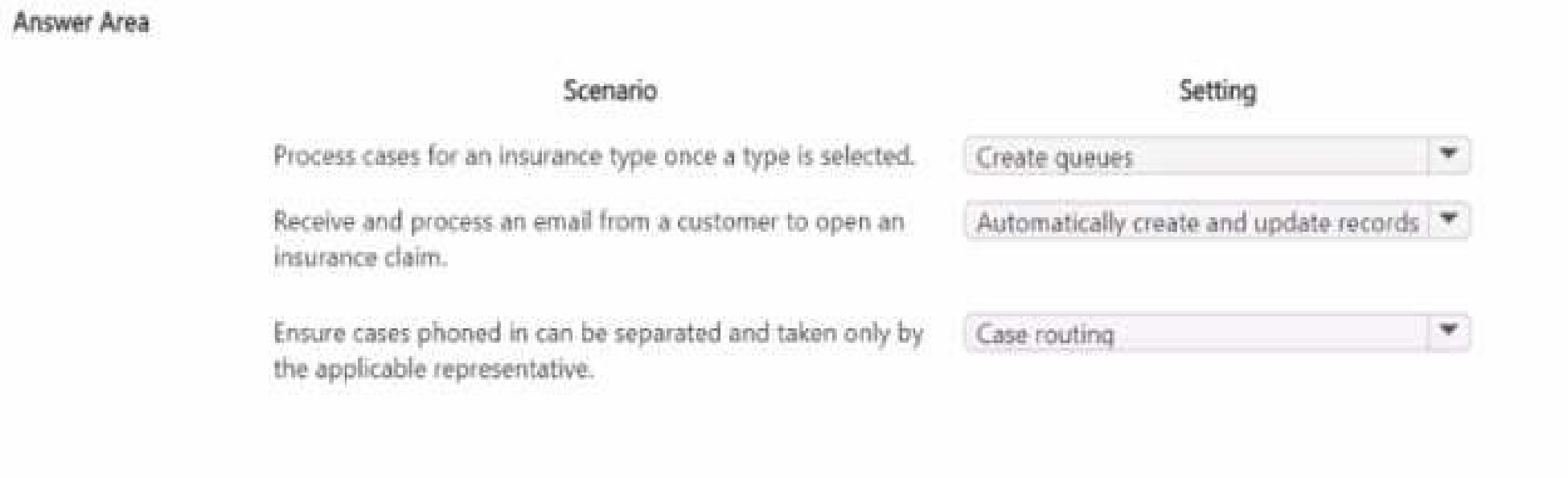
Which settings should you configure? To answer, select the appropriate options in the answer area.
NOTE: Each correct selection is worth one point.

Microsoft Dynamics 365 Customer Service Functional Consultant Practice test unlocks all online simulator questions
Thank you for choosing the free version of the Microsoft Dynamics 365 Customer Service Functional Consultant practice test! Further deepen your knowledge on Microsoft Simulator; by unlocking the full version of our Microsoft Dynamics 365 Customer Service Functional Consultant Simulator you will be able to take tests with over 327 constantly updated questions and easily pass your exam. 98% of people pass the exam in the first attempt after preparing with our 327 questions.
BUY NOWWhat to expect from our Microsoft Dynamics 365 Customer Service Functional Consultant practice tests and how to prepare for any exam?
The Microsoft Dynamics 365 Customer Service Functional Consultant Simulator Practice Tests are part of the Microsoft Database and are the best way to prepare for any Microsoft Dynamics 365 Customer Service Functional Consultant exam. The Microsoft Dynamics 365 Customer Service Functional Consultant practice tests consist of 327 questions and are written by experts to help you and prepare you to pass the exam on the first attempt. The Microsoft Dynamics 365 Customer Service Functional Consultant database includes questions from previous and other exams, which means you will be able to practice simulating past and future questions. Preparation with Microsoft Dynamics 365 Customer Service Functional Consultant Simulator will also give you an idea of the time it will take to complete each section of the Microsoft Dynamics 365 Customer Service Functional Consultant practice test . It is important to note that the Microsoft Dynamics 365 Customer Service Functional Consultant Simulator does not replace the classic Microsoft Dynamics 365 Customer Service Functional Consultant study guides; however, the Simulator provides valuable insights into what to expect and how much work needs to be done to prepare for the Microsoft Dynamics 365 Customer Service Functional Consultant exam.
BUY NOWMicrosoft Dynamics 365 Customer Service Functional Consultant Practice test therefore represents an excellent tool to prepare for the actual exam together with our Microsoft practice test . Our Microsoft Dynamics 365 Customer Service Functional Consultant Simulator will help you assess your level of preparation and understand your strengths and weaknesses. Below you can read all the quizzes you will find in our Microsoft Dynamics 365 Customer Service Functional Consultant Simulator and how our unique Microsoft Dynamics 365 Customer Service Functional Consultant Database made up of real questions:
Info quiz:
- Quiz name:Microsoft Dynamics 365 Customer Service Functional Consultant
- Total number of questions:327
- Number of questions for the test:50
- Pass score:80%
You can prepare for the Microsoft Dynamics 365 Customer Service Functional Consultant exams with our mobile app. It is very easy to use and even works offline in case of network failure, with all the functions you need to study and practice with our Microsoft Dynamics 365 Customer Service Functional Consultant Simulator.
Use our Mobile App, available for both Android and iOS devices, with our Microsoft Dynamics 365 Customer Service Functional Consultant Simulator . You can use it anywhere and always remember that our mobile app is free and available on all stores.
Our Mobile App contains all Microsoft Dynamics 365 Customer Service Functional Consultant practice tests which consist of 327 questions and also provide study material to pass the final Microsoft Dynamics 365 Customer Service Functional Consultant exam with guaranteed success. Our Microsoft Dynamics 365 Customer Service Functional Consultant database contain hundreds of questions and Microsoft Tests related to Microsoft Dynamics 365 Customer Service Functional Consultant Exam. This way you can practice anywhere you want, even offline without the internet.
BUY NOW